Overview
Warning signs of a bedsore

Warning signs of a bedsore
Relieve pressure on an area that is showing signs of being stressed.
Bedsore
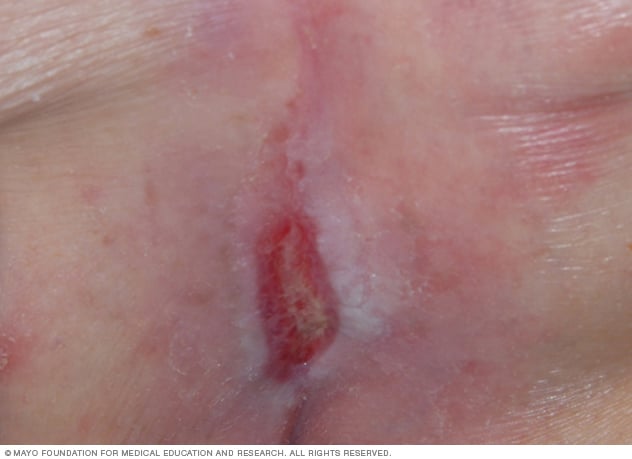
Bedsore
Bedsores are areas of damaged skin and tissue caused by sustained pressure — often from a bed or wheelchair — that reduces blood circulation to vulnerable areas of the body.
Bedsores — also called pressure ulcers and decubitus ulcers — are injuries to skin and underlying tissue resulting from prolonged pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such as the heels, ankles, hips and tailbone.
People most at risk of bedsores have medical conditions that limit their ability to change positions or cause them to spend most of their time in a bed or chair.
Bedsores can develop over hours or days. Most sores heal with treatment, but some never heal completely. You can take steps to help prevent bedsores and help them heal.
Products & Services
Symptoms
Warning signs of bedsores or pressure ulcers are:
- Unusual changes in skin color or texture
- Swelling
- Pus-like draining
- An area of skin that feels cooler or warmer to the touch than other areas
- Tender areas
Bedsores fall into one of several stages based on their depth, severity and other characteristics. The degree of skin and tissue damage ranges from changes in skin color to a deep injury involving muscle and bone.
Common sites of pressure ulcers
For people who use wheelchairs, bedsores often occur on skin over the following sites:
- Tailbone or buttocks
- Shoulder blades and spine
- Backs of arms and legs where they rest against the chair
For people who need to stay in bed, bedsores may happen on:
- The back or sides of the head
- The shoulder blades
- The hip, lower back or tailbone
- The heels, ankles and skin behind the knees
When to see a doctor
If you notice warning signs of a bedsore, change your position to relieve the pressure on the area. If you don't see improvement in 24 to 48 hours, contact your doctor.
Seek immediate medical care if you show signs of infection, such as a fever, drainage from a sore, a sore that smells bad, changes in skin color, warmth or swelling around a sore.
Causes
Bedsores are caused by pressure against the skin that limits blood flow to the skin. Limited movement can make skin vulnerable to damage and lead to development of bedsores.
Three primary contributing factors for bedsores are:
-
Pressure. Constant pressure on any part of your body can lessen the blood flow to tissues. Blood flow is essential for delivering oxygen and other nutrients to tissues. Without these essential nutrients, skin and nearby tissues are damaged and might eventually die.
For people with limited mobility, this kind of pressure tends to happen in areas that aren't well padded with muscle or fat and that lie over a bone, such as the spine, tailbone, shoulder blades, hips, heels and elbows.
- Friction. Friction occurs when the skin rubs against clothing or bedding. It can make fragile skin more vulnerable to injury, especially if the skin is also moist.
- Shear. Shear occurs when two surfaces move in the opposite direction. For example, when a bed is elevated at the head, you can slide down in bed. As the tailbone moves down, the skin over the bone might stay in place — essentially pulling in the opposite direction.
Risk factors
Your risk of developing bedsores is higher if you have difficulty moving and can't change position easily while seated or in bed. Risk factors include:
- Immobility. This might be due to poor health, spinal cord injury and other causes.
- Incontinence. Skin becomes more vulnerable with extended exposure to urine and stool.
- Lack of sensory perception. Spinal cord injuries, neurological disorders and other conditions can result in a loss of sensation. An inability to feel pain or discomfort can result in not being aware of warning signs and the need to change position.
- Poor nutrition and hydration. People need enough fluids, calories, protein, vitamins and minerals in their daily diets to maintain healthy skin and prevent the breakdown of tissues.
- Medical conditions affecting blood flow. Health problems that can affect blood flow, such as diabetes and vascular disease, can increase the risk of tissue damage such as bedsores.
Complications
Complications of pressure ulcers, some life-threatening, include:
- Cellulitis. Cellulitis is an infection of the skin and connected soft tissues. It can cause warmth, inflammation and swelling of the affected area. People with nerve damage often do not feel pain in the area affected by cellulitis.
- Bone and joint infections. An infection from a pressure sore can burrow into joints and bones. Joint infections (septic arthritis) can damage cartilage and tissue. Bone infections (osteomyelitis) can reduce the function of joints and limbs.
- Cancer. Long-term, nonhealing wounds (Marjolin's ulcers) can develop into a type of squamous cell carcinoma.
- Sepsis. Rarely, a skin ulcer leads to sepsis.
Prevention
You can help prevent bedsores by frequently repositioning yourself to avoid stress on the skin. Other strategies include taking good care of your skin, maintaining good nutrition and fluid intake, quitting smoking, managing stress, and exercising daily.
Tips for repositioning
Consider the following recommendations related to repositioning in a bed or chair:
- Shift your weight frequently. Ask for help with repositioning about once an hour.
- Lift yourself, if possible. If you have enough upper body strength, do wheelchair pushups — raising your body off the seat by pushing on the arms of the chair.
- Look into a specialty wheelchair. Some wheelchairs allow you to tilt them, which can relieve pressure.
- Select cushions or a mattress that relieves pressure. Use cushions or a special mattress to relieve pressure and help ensure that your body is well positioned. Do not use doughnut cushions, as they can focus pressure on surrounding tissue.
- Adjust the elevation of your bed. If your bed can be elevated at the head, raise it no more than 30 degrees. This helps prevent shearing.
Tips for skin care
Consider the following suggestions for skin care:
- Keep skin clean and dry. Wash the skin with a gentle cleanser and pat dry. Do this cleansing routine regularly to limit the skin's exposure to moisture, urine and stool.
- Protect the skin. Use moisture barrier creams to protect the skin from urine and stool. Change bedding and clothing frequently if needed. Watch for buttons on the clothing and wrinkles in the bedding that irritate the skin.
- Inspect the skin daily. Look closely at your skin daily for warning signs of a pressure sore.